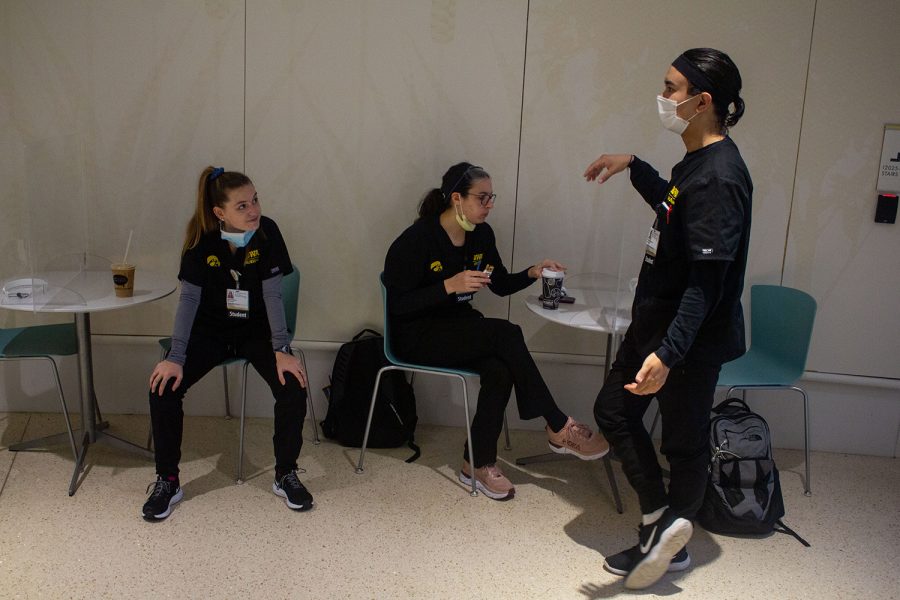Health care professionals remain vigilant, resilient after a year on the frontlines of the COVID-19 pandemic
When Iowa saw 340,000 COVID-19 cases and more than 5,000 deaths in the last year, health care professionals at UIHC remained resilient.
University of Iowa senior and undergraduate BSN nursing student, Nick Figuracion (right), and fellow nursing students, Amy Gustafson (left) and Rebecca Sandhu (center), talk before their clinical rotation on Thursday, March 11 in the University of Iowa Stead Family Children’s Hospital. Figuracion’s advice to other nursing students during COVID is that, “You have to persevere. These times are tough for everyone and none of this is natural to us. Wearing masks and face shields and standing six feet apart that’s not human. Human interaction is being close and interacting with one another, so you just have to persevere and know that there is light at the end of the tunnel.”
March 16, 2021
Jess Shever is exhausted.
A year after the first case of novel coronavirus was discovered in Johnson County, Shever said there is an added emotional toll on her and her colleagues to do their jobs during the pandemic. Because visitors aren’t allowed in the hospital to minimize the spread of COVID-19, the responsibility of supporting patients and contacting family members for an over-the-phone visit adds more day-to-day work and emotional energy, said Shever.
Shever is a staff nurse in the Medical intensive-care unit at the University of Iowa Hospitals and Clinics, which has served as ground zero for COVID-19 patients over the last year.
“I know several of my colleagues were in the room when patients died at the beginning when we weren’t allowing anyone to come in,” she said. “The nurses stay in the room and hold their hand and tell them it’s OK to die and that happens every once in a while prior to the pandemic, but it was just happening with such increased frequency. It takes a big emotional toll and it’s challenging.”
Health care workers have been on the frontlines of the COVID-19 pandemic and haven’t gotten a break, said Shever, who hasn’t taken a vacation in six months. UIHC implemented two-week long furloughs for its employees to assist in millions of dollars in COVID-19 losses in June 2020.
Shever decided to split her furlough in half — taking one week off and working the other — after witnessing the impact furloughs had on her unit. She said she has had to add to her self-care routine to ensure she can continue working — and she isn’t alone.
Anne Sullivan, an occupational therapist who has worked for UIHC for eight years, said the stress from the pandemic has severely impacted her mental and emotional wellbeing, so she’s also leaning on a routine to help her continue working.
“Burnout is real and I see it affecting a lot of my colleagues,” Sullivan said. “I’ve made a point to do as much self-care as possible by resting, exercising, and eating…[COVID-19] hurts your heart. And it adds another layer of exhaustion, so we have to take care of ourselves.”
RELATED: Nurse liaisons provide human connection, technology support to patients
Both Sullivan and Shever said they’ve focused on ensuring they have time to take care of themselves during the pandemic to decrease the stress of their day-to-day jobs. They’ve seen their colleagues do the same.
From June to September 2020, Mental Health America surveyed 1,119 health care workers from various states about their mental health during the COVID-19 pandemic. The organization found that 76 percent of the survey’s respondents reported exhaustion and burnout and 82 percent said they were emotionally exhausted.
Sullivan said she can’t believe it’s already been a year since Iowa identified its first COVID-19 cases and deaths. She called the beginning of the pandemic terrifying because more questions circled than answers when it came to protection while working in a hospital.
At first, she said she didn’t know what protective equipment to wear and where the gear would be coming from. Not knowing how to protect herself, her colleagues, and her patients was one of the hardest things she’s had to do, Sullivan said.
“When the pandemic started, it was scary,” she said. “So much was unknown when it came to protocols and what PPE to wear and the availability of protective gear. We were on edge when it came to work safety.”
While UIHC is lucky to have enough personal protective equipment for all of its employees, Sullivan said it is challenging and exhausting when it comes to communicating with patients. She said she often has to yell for patients to understand her.
As an occupational therapist, Sullivan works with patients of all ages with any condition to recuperate and recover daily skills. She said she has worked with some hard-of-hearing patients during the pandemic where communication was a barrier before the pandemic, and has only gotten worse with the layers of masks and face shields.
Health care workers, however, are not the only handling the pandemic, but dealing with a nursing shortage across the country.
RELATED: University of Iowa Hospitals and Clinics uses temporary nurses to fill gaps
Sullivan said several qualified nurses who have spent their lives serving patients have left UIHC during the pandemic. While none have left her unit specifically, she said losing nurses has been difficult for other units.
At a bargaining session with the state Board of Regents in January, SEIU 199, the union that serves health care workers like Sullivan, said there were several underlying factors when it came to nurses leaving UIHC, including scheduling problems and the expense of traveling nurses.
As The Daily Iowan previously reported, UIHC is using traveling nurses to fill the gaps within its workforce. The UI, however, is working to help combat the shortage of trained nurses within its College of Nursing, said associate dean for undergraduate programs at the UI’s College of Nursing, Anita Nicholson.
“At the College of Nursing, we’re preparing nurses to graduate and get out into the field and help with the shortage,” she said. “We graduate students twice a year through two tracks – pre licensure and RN BSN. Our program is working to navigate the COVID crisis and ensure graduates are prepared to provide quality nursing care and navigate the complex health care field.”
Moving forward, Sullivan said she is looking forward to having visitors in the hospital again. UIHC added several precautions at the beginning of the pandemic to decrease the spread of COVID-19, including postponing all visitors for adult patients in April 2020.
As the spread of the coronavirus slows and more individuals are vaccinated, Sullivan said she is looking forward to seeing more people in the hospital and adding visitor education back into her everyday work.
“I’m ready for normalcy and for people to have visitors,” she said. “I appreciate the strict visitor policy because it’s keeping people safe and I’m glad the university has done that, but a big part of my job is family caregiver education, so I look forward to being able to do that in person.”
As she looks forward, Shever said she is excited to see her family now that she’s been vaccinated. She said that though the end of the pandemic is coming, it isn’t here yet and encouraged people to continue wearing masks and to get their vaccinations when it’s available to them.
“The university community overall has been supportive of following social distancing and wearing masks and that’s been great,” she said. “But it’s been a struggle, sometimes, to listen to our governor implement different non strategies to mitigate the spread of COVID…The end is coming, but it’s not here yet.”
While this year has been long and grueling for health care professionals on the front lines, Sullivan said it is an experience she will never forget.
“This past year, there has been so much sadness, grief, and heartbreak when it comes to taking care of our patients,” Sullivan said. “I applaud the nurses I work with and the other therapists, because we’ve had to pick up more of the emotional load that normally family members would have when supporting their loved ones.”