Vaccine experts say ‘don’t let guard down’ after getting COVID-19 vaccine
And other answers to questions about the COVID-19 vaccines in Iowa.
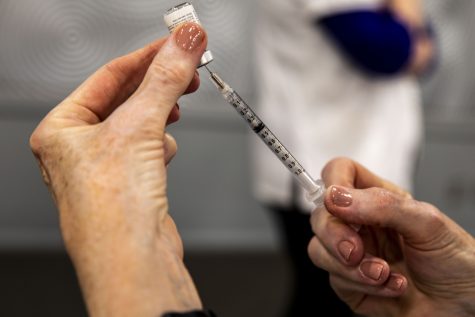
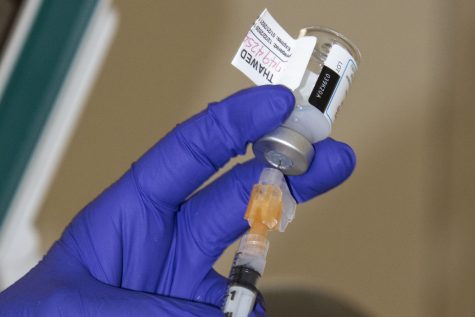
A member of UIHC staff fills needles with the Moderna vaccine on Friday, Jan. 29, 2021 at the UI Medical Education Research Facility.
As Iowa ramps up its distribution of the COVID-19 vaccine, The Daily Iowan sat down with vaccine trial lead and Executive Dean of the University of Iowa Carver College of Medicine Patricia Winokur to answer questions about the vaccines available, their effectiveness, and new strains of COVID-19.
Iowa ranks near the middle of all other states for percent of population with the first dose administered, with 13.6 percent of the state receiving the first dose, according to the Washington Post’s vaccine tracker, but fourth from last in completed vaccination, at 4.5 percent of the state’s population.
Iowa has two vaccines available — Moderna and Pfizer — to people ages 65 and older and in addition to people in high-risk professions. The Iowa Department of Public Health put together a priority group recommendation for people to receive the vaccine.
Currently health care workers, first responders, K-12 education staffers, agriculture distribution and manufacturing workers, individuals with disabilities in group home settings, those living in congregate settings (not including college residence halls), government officials, health- and child-safety inspectors and correctional facility staff, and individuals incarcerated are eligible for the vaccine in a five-tiered system of priority.
Iowa is delivered an allotment of vaccines from the federal government, Winokur said, which is then distributed to county public health departments and allocated to health care facilities and other vaccine distributors in the county. In Johnson County, UI Health Care, Mercy Iowa City, and some area pharmacies are offering appointments for the vaccine, though a decentralized process has meant difficult planning and spurious appointments for Iowans. Iowa City Veterans Affairs hospital doles out a separate federal allotment of the vaccine to area veterans.
How does the vaccine work?
The Pfizer and Moderna vaccines, the two approved for emergency authorization by the FDA as of now, are called mRNA vaccines. Explained in basic terms by the Centers for Disease Control and Prevention, mRNA is instructions for the cell on how to make part of the spike protein that prompts the immune system to make antibodies that fight against a future coronavirus infection.
“So, the vaccines that we have that we’re evaluating in the United States and those that we have emergency-use authorization — all are based off of showing your immune system the spike protein,” Winokur said. “And the spike protein is that protein that sits on the outside of the coronavirus, and that’s the main protein that your immune system recognizes to develop antibodies and other cells that protect you from future infections.”
Winokur said one myth about the COVID-19 vaccine is that the vaccine changes your DNA — it doesn’t. After the spike protein is made, the cell breaks down and disposes of the mRNA strand, and never enters the cell’s nucleus or affects genetic material.
Could I still be infected by COVID-19 if I’ve had one or both doses of a vaccine?
The Pfizer and Moderna vaccines both near 95-percent effectiveness in preventing symptomatic COVID-19, Winokur said, and there are early indications that the vaccines also prevent transmission.
“It [the vaccine] is probably preventing infections completely,” Winokur said. “The data is still being worked out. We know it prevents people from getting symptomatic COVID-19 — that was the primary endpoint that the FDA wanted the companies to show. That’s where the 95-percent efficacy is. But we’re starting to get inklings of different ways that we are seeing that it reduces infections as well.”
About two weeks after the first dose, the vaccine is between 60-80 percent effective, Winokur said. But the second dose seals the 95 percent effectiveness.
What about with the COVID-19 variants, such as ones prominent in the U.K. or South Africa?
Iowa confirmed cases of a more easily transmissible variant of the coronavirus from the U.K. earlier this month. Winokur said, as researchers have gathered preliminary data from vaccine distribution in South Africa, where another variant is prominent, vaccines seem to be less effective.
For example, Winokur said, researchers found one vaccine from Johnson and Johnson that is expected to receive emergency authorization in the coming weeks to be in the 72-percent efficacy range when tested in the U.S. That efficacy dropped into the low 60-percent range in South Africa, however.
“The vaccines have less efficacy in the South African region where this variant is prominent,” Winokur said. “It is not complete — they still have some efficacy, but it is not as good as against the original strains that were the targets for those vaccines.”
She emphasized, though, that the Johnson and Johnson vaccine still did a good job of preventing severe illness from COVID-19. During surges of severe COVID-19 cases, hospitals have warned that too many patients in the ICU can overwhelm health care facilities and result in preventable deaths.
When will I be able to hug my loved ones who are at risk?
The date of returning to “normalcy” is elusive, Winokur said. Anthony Fauci, Biden’s chief medical adviser, told CNN to expect a “significant degree of normality” by fall, but that people could still be expected to wear face masks in public as long as a year from now.
Public health experts have said that, to squelch the pandemic, the country would need to reach herd immunity, which is when a large enough share of the population is immune to the virus to prevent transmission.
For people who have been vaccinated, Winokur said public health experts are recommending the continuation of wearing masks to curb the spread of variants and normalization of masking.
“What we are telling people who have been vaccinated is don’t let your guard down,” she said. “Remember, not everybody is vaccinated, you are setting yourself up as a role model.”
Where can I get the vaccine?
Iowa health officials have warned that there is not enough vaccine for everyone eligible to be vaccinated in priority group 1B right now. Anyone in Iowa can fill out a form on the UIHC website to express interest in receiving the vaccine. Mercy Iowa City is distributing the vaccine to those eligible by contacting eligible patients.
According to the Iowa Department of Public Health website, there are eight locations not including UIHC or Mercy that offer the vaccine. Six are area Hy-Vees and two — North Liberty Pharmacy and Towncrest Pharmacy — are local pharmacies.
As of Sunday afternoon, Iowa City and Cedar Rapids Hy-Vee locations had no appointments available online. CVS pharmacy, too, offers but did not have any appointments available for COVID-19 vaccines at its Cedar Rapids location.
Debunking COVID-19 vaccine myths
No, the vaccine does not cause fertility issues and no, the vaccine does not change your DNA, Winokur said of two vaccine myths she’s seen circling the internet.
“We have done animal studies looking at fertility, and we now have vaccines that have gone out into the population,” Winokur said. “About 20,000 women who are pregnant have gotten the vaccine, and we have not seen any problems with those pregnancies.”
She added, as for the DNA-changing myth, the mRNA is broken down so quickly it won’t get into any coding areas of the body.
“One of the nice things about these messenger RNA vaccines is the messenger RNA is very transient. It is destroyed very quickly.”
What if I have a pollen allergy? Should I still get the vaccine?
Allergic reaction to a COVID-19 vaccine is very rare, Winokur said, and the few recorded cases have been in people who had a history of anaphylaxis, a severe allergic reaction. About 60 cases have been reported in the U.S., and there’s not a risk to people with pollen or ragweed allergies.
“Seasonal allergies to ragweed or pollen — those are not the types of allergic histories that make us most worried,” Winokur said. “It’s really people who’ve had anaphylaxis to different compounds — and especially if you’ve had anaphylaxis to a previous vaccine.”

(she/her/hers)
Email: [email protected]
Twitter: @K_5mydearwatson
Sarah Watson is the executive editor at The Daily Iowan. She's in her...

(she/her/hers)
Email: [email protected]
Hannah Kinson is the Photo Assistant Visuals Editor at The Daily Iowan. Hannah is a senior majoring in...