Black leaders, public health experts look to build trust in COVID-19 vaccine
Black Americans are disproportionately affected by the pandemic. Now, public health leaders must overcome a history of cultural trauma that sows mistrust in a vaccine.
President and CEO at MYEP Roger Lusala poses for a portrait on Monday, Dec. 14, 2020 in his office at MYEP.
December 15, 2020
Some of Roger Lusala’s close friends and family — even his kids — raised eyebrows when he told them this summer he’d take part in a COVID-19 vaccine trial.
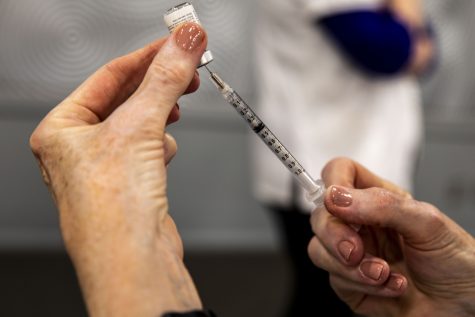
The Pfizer-BioNtech vaccine, approved last week and delivered to front-line health care workers Monday, is 95 percent effective in preventing the deadly disease, but Lusala didn’t know that at the time.
He pointed to the medical communities’ rigorous examination process, and Pfizer’s refusal of federal funding in early research stages, as part of the reason he trusted the UI to participate in the two-year study.
“When you get a prescription, no one ever goes to the lab and crushes the medication and studies it. You trust your doctor,” he said. “You have so many scientific professionals studying this. So, we have to trust the science.”
When Lusala’s doctor contacted him about the Pfizer-BioNtech vaccine trial, the local site at the University of Iowa Hospitals and Clinics, he knew that the 40,000-plus person study needed people who looked like him to be most accurate. As a Black community leader, he could provide testimony to a group of people that has historically been mistrustful of medicine — and has good reason to be.
“A vaccine would help everybody, and especially, I wanted to do it for the Black community so I can testify to let them know that I was part of that,” said Lusala, who came to the U.S. in 1992 from the Democratic Republic of Congo. “So nobody has to be afraid.”
Lusala, CEO of an Iowa City-based disability-services agency and Iowa City Human Rights Commission member, was part of a blinded study, meaning he won’t know until the vaccine is available to the public whether he received the placebo or the actual vaccine.
“I took it and I haven’t changed,” he said. “I haven’t had any side effects. I hope I got the vaccine, but if I didn’t, I will be first in line to get one.”
As the first doses of a two-dose vaccine arrive in hospitals nationwide, Iowa public health experts are trying to build trust in a vaccine among Black communities through trusted messengers like Lusala.
Fewer than half of Black Americans say they would get a coronavirus vaccine, compared with 63 percent of Hispanic people and 61 percent of white people, according to a December survey from the Pew Research Center — and there is a history behind that mistrust, Iowa-Nebraska NAACP health equity chair Jacqueline Easley McGhee said.
“African Americans have long been medical guinea pigs for so-called scientific experimentation,” Easley McGhee said. “So there’s that longstanding mistrust and add to that you’re getting all stories from the federal government. Do they have our best interests in mind? Was it too hasty? Was it politically motivated? As a health care professional, I can understand the concern and the questions.”
In 1932, the Public Health Service started a study with the Tuskegee Institute to document syphilis in Black people. Researchers told participants in the study, which went on for four decades, that they were receiving experimental treatment. In truth, researchers allowed the disease to run its course until people with syphilis died.
After undergoing treatment for cervical cancer at John Hopkins’ Hospital in 1951, Henriettta Lacks’ cells were cultivated without her consent for research. Now, there are more than 17,000 patents with so-called HeLa cells, including in COVID-19 vaccine research.
The “father” of gynecology developed modern practices used today — such as the speculum and the Sims position — by experimenting on enslaved Black women without using anesthesia.
As the health equity chair of the Iowa-Nebraska NAACP, Easley McGhee is passionate about health equity outcomes for people of color and works around the clock to get the word out about preventative health measures for those who are disproportionately impacted by the virus.
RELATED: University of Iowa Hospitals and Clinics prepares for COVID-19 vaccine expected in November
She said several questions will need to be clearly addressed in order to have the highest participation rate possible from the Black community.
What are the logistics of a vaccine rollout and its accessibility? Of the 40,000+ people who participated in the Pfizer trial, how many were Black or people of color?
Cost and distribution to the general public still remain question marks locally, said Susan Vileta, a health educator with Johnson County Public Health. A top Pfizer executive this fall said about a fifth of the participants enrolled in August were Hispanic or Black, two groups hit hardest by COVID-19.
In Iowa, UIHC received 1,000 initial doses on Monday to distribute to its front line COVID-19 staff.
Easley McGhee hopes to provide the answers through trusted communication channels in order to build credibility of a vaccine’s safety and effectiveness in Black communities.
“It’s important for people to hear from experts who look like them,” Easley McGhee said. “It will, in some ways, increase confidence that the vaccine will be safe.”
She plans to host a Facebook Live town hall with a panel of national Black health experts — including an infectious disease expert from Howard University — to answer questions. It’s also important to do outreach to faith leaders with public health messaging, Easley McGhee said, to make inroads in Black communities.
Johnson County Public Health and UIHC leaders are planning a massive public health campaign to promote the rollout of the vaccine and including community leaders to distribute accurate information.
JCPH partners with organizations such as Nisaa, the local African Family Services chapter, and works closely with Congolese Health Partnership. One JCPH manager speaks French, Vileta said, and helps to translate important health information for people who’ve come to the U.S. from the Democratic Republic of Congo living in Johnson County.
Vaccines train immune systems to create proteins that fight disease, known as antibodies. That is the same process as would happen when people are exposed to a disease but – importantly – vaccines work without making people very sick. It’s unclear yet if any COVID-19 vaccine stops transmission or “shedding” of the virus, according to the CDC, but the Pfizer-BioNtech vaccine is 95 percent effective in preventing COVID-19 infection.
If enough Americans are vaccinated, the country can reach so-called “herd immunity” which would mean enough people would be immune to the virus that those who can’t receive a vaccine for health and immunity-compromising reasons would be relatively safe.
“If we don’t have every group in our community on board those numbers aren’t going to be high enough to get us the protection that we need,” Vileta said.
UIHC does not yet know whether it will be a site for the public to receive a vaccine, UIHC CEO Suresh Gunasekaran told reporters last week. But, if it does, accessibility and ease of being vaccinated will be key hurdles in making sure as many people as possible can receive the vaccine.
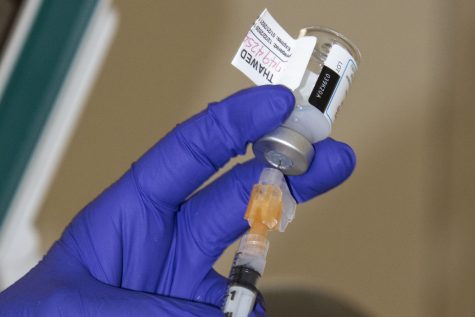
The Pfizer-BioNtech vaccine must be kept at sub negative 70 degrees Celsius and must be used soon after it thaws, complicating delivery. Plus, people will have to receive two doses, making logistics more complicated than an average one-dose flu vaccine.
“This Pfizer first candidate just logistically, it gets harder. It’s harder to make this a mobile vaccination unit., it’s harder to distribute it,” Gunasekaran said. “…. We want to work with community-based health workers, we want to work with community-based organizations that these communities trust, and hopefully we can figure out a delivery mechanism as to how we can pair a vaccination program with that.”
Underrepresented ethnic and racial groups have been disproportionately hit by the virus nationwide, a result of decades of being more likely to have underlying conditions and working in high-risk environments, making distribution to those groups all the more important. Easley McGhee was key in prodding Iowa’s state government to begin releasing a breakdown of COVID-19 data by race and ethnicity to be aware of these disparities.
At the time the data was first released in April, Black and Hispanic Iowans were disproportionately testing positive for the virus in the Hawkeye State. According to the U.S. Census Bureau, Black Iowans make up about 4 percent of Iowa’s population, but made up 8.7 percent of those who tested positive for the virus, according to information released in April.
Hispanic and Latino Iowans fared worse — making up 6.2 percent of the state, but representing 16.4 percent of the population that tested positive at the time.
Since then, the data in Iowa has evened out between races, though it’s difficult to draw conclusions as 32 percent of those who tested positive are in a category of “unknown” for race/ethnicity. About 3 percent of positive tests were African Americans.
Disparities do not carry over to deaths. African Americans account for 2.63 percent of deaths and whites account for 91.73 percent of COVID-19 deaths.
“The pandemic was a Band-Aid that was ripped off of a festering wound of health inequity,” Easley McGhee said.