Iowa hospitals face mounting financial pressure, stagnating Medicaid reimbursement
After the city of Keokuk lost its community hospital, residents must travel almost half an hour for emergency medical care. It is one of a number of hospitals in the state struggling to stay afloat.
April 23, 2023
Among the hills of the Mississippi River valley in the southeastern tip of Iowa lies the quaint city of Keokuk. The town of just under 10,000 residents is one of many rural communities that has lost a core service — its community hospital.
In October 2022, Blessing Health Keokuk closed its doors to inpatient and emergency room care while keeping its family medicine clinic open.
Officials at the 71-bed hospital said it wasn’t getting enough business to sustain operations at the facility that it bought in March of 2021 — just a year and nine months before it closed its doors.
According to data collected by the National Center for Healthcare Quality and Payment Reform, Blessing Health’s Keokuk facility was in the red, spending 13 percent more than expected revenue in its last year of operation.
Keokuk Mayor Kathie Mahoney told The Daily Iowan that after the facility closed, residents worried about accessibility to care when needed. With the closest hospital 18 miles away and a 30-minute drive in Fort Madison, many residents are worried help might not be available in time if an emergency strikes. There are no other emergency care facilities in Keokuk city limits.
“We’ve always had a hospital here,” Mahoney said. “If you had any problems, you were capable of getting to a facility within a couple of minutes.”
In addition to the hospital closing, Lee County emergency medical services, the ambulance service for the entire county, has limited resources. With only two or three ambulances operating during any given time and longer transport times because of the hospital closure, Mahoney worries some residents might have to wait longer for emergency care.
For the time being, Mahoney said, the Keokuk Fire Department provides emergency care if an ambulance isn’t available in time but is unable to transport patients.
Mahoney said Lee County is looking into purchasing a fourth ambulance to increase emergency medical response availability and decrease wait times for emergency care.
Lee County first responders did not respond to a request for comment.
Recently, the Keokuk community has opened its arms to Insight Healthcare and signed a letter of intent to acquire the hospital from Blessing Health. The company signed a letter of intent in January, Mahoney said.
Blessing Health Keokuk isn’t the only rural hospital facing financial pressures, and Keokuk isn’t the only small town in America that has lost its community hospital.
According to data from the National Center for Healthcare Quality and Payment Reform, 188 rural hospitals have closed their doors nationwide since 2005, and 220 are at immediate risk of closing. Rural hospitals are classified by the U.S. Department of Health and Human Services and serve communities designated rural by the U.S. Census.
In Iowa, Blessing Health Keokuk is the only rural hospital to close since 2005, but 24 percent of rural hospitals in the state are at risk of closing, two of which are at immediate risk of closure.

Dr. Brent Hoehns types on a computer at the Knoxville Hospital and Clinics in Knoxville, Iowa on Tuesday, March 14, 2023. Hoehns has been a doctor for 28 years and sees the benefits of working in a smaller hospital. “It’s big enough that you can have eight or 10 partners, but small enough that you get to know the administration. You get a lot more say in how things are run than if you’re one of a thousand physicians in a system,” Hoehns said.
Rural hospitals under financial crunch
Iowa Hospital Association President and CEO Chris Mitchell said stagnant Medicaid reimbursement rates are hurting rural hospitals and leaving them in financial jeopardy. As legislators attempt to steady the financial headwinds for rural hospitals, Medicaid reimbursement rate increases have not gained bipartisan support.
Most of Iowa’s rural hospitals are losing money on providing patient care, but some hospitals remain financially afloat because of local tax levies and federal grants, according to the National Center for Healthcare Quality and Payment Reform. More than 9 percent of Iowa hospitals are operating in the red, according to the CHQPR.
Mitchell said stagnant Medicaid and Medicare payment rates to hospitals are affecting their ability to stay in the black on operating costs. Iowa’s Medicaid reimbursement rates for providers haven’t increased in a decade, Mitchell said.
Mitchell said 10 percent of Iowa hospitals have unsustainable operating margins, where the total cost of patient care is more than the amount of revenue from insurance payments.
According to Kaiser Health, 20 percent of Iowans are covered by the state’s Medicaid program.
The stagnation of Medicaid reimbursement rates is coupled with rising costs increased financial stress on Iowa’s hospitals. Approximately 61 percent of Iowa hospitals operate with a negative patient services margin, meaning they lose money on providing care, Mitchell said.
The Iowa Department of Health and Human Services announced in March that it would begin reevaluating Medicaid enrollees in the state and requiring them to reapply to keep services after this practice was paused because of COVID-19. Under the new program, 100,000 Iowans will be eventually unenrolled from the state’s Medicaid system, leaving many without insurance, according to the Des Moines Register.
“That is a direct result of the lack of reimbursement from the three major payers [Medicaid, Medicare, and private insurance],” Mitchell said. “When hospitals are facing these sorts of [financial] pressures, there’s not a whole lot of levers they have to pull.”
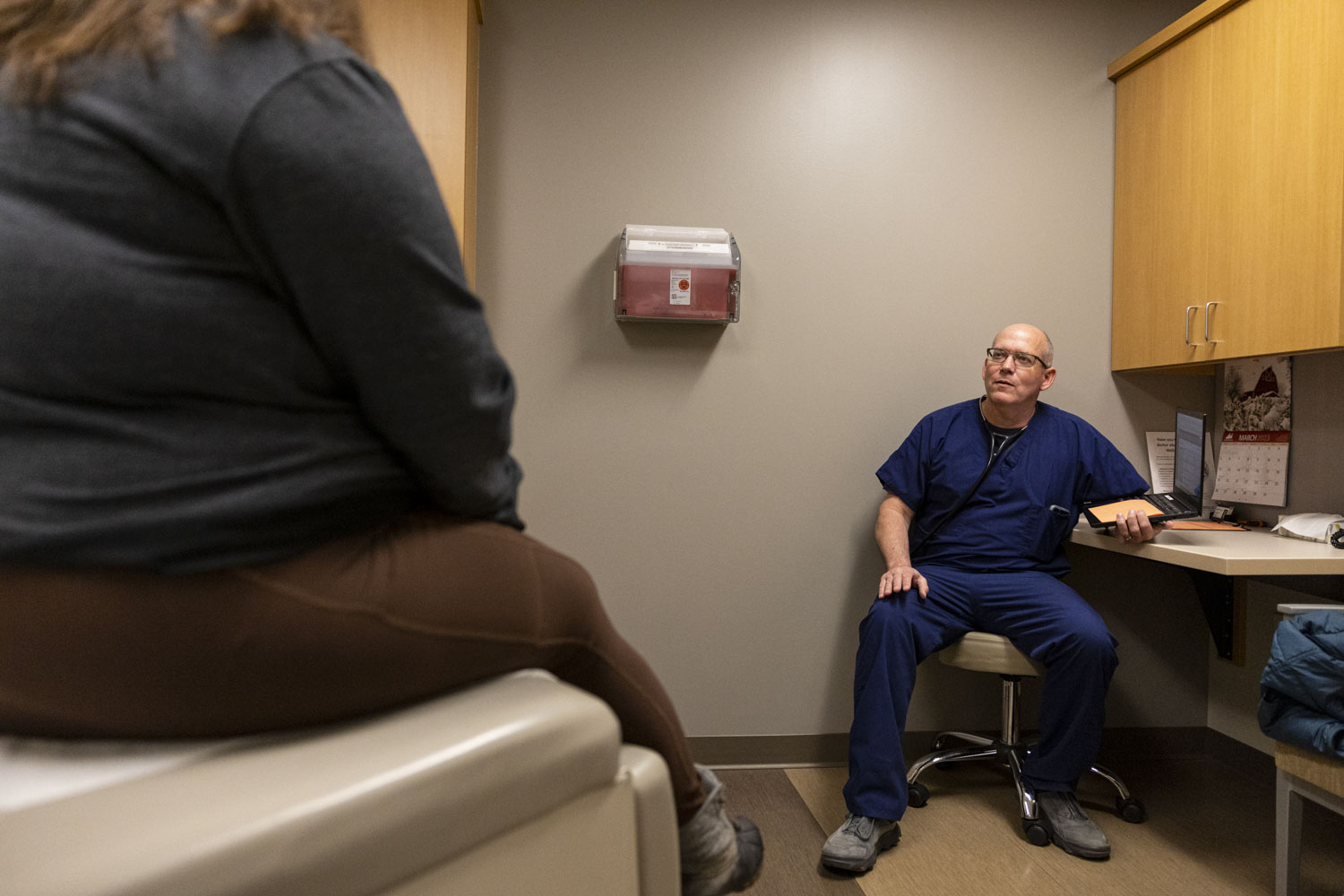
Dr. Brent Hoehns talks with a patient at the Knoxville Hospital and Clinics in Knoxville, Iowa on Tuesday, March 14, 2023. Hoehns has been a doctor for 28 years and sees the benefits of working in a smaller hospital. “It’s big enough that you can have eight or 10 partners, but small enough that you get to know the administration. You get a lot more say in how things are run than if you’re one of a thousand physicians in a system,” Hoehns said.
Lawmakers seek lifeline for rural hospitals
The Iowa Legislature has worked to address the financial pressure that rural hospitals face, though some say policymakers’ solutions haven’t gone far enough to give the facilities the lifelines they need to stay open.
Iowa Gov. Kim Reynolds signed Senate File 75 into law on March 28 and established a state licensure process allowing certain hospitals to receive a Rural Emergency Hospital designation. Hospitals with this designation would have to cease inpatient care and surgical procedures. Under the license, the hospital would not be able to provide care for a patient longer than 24 hours.
The designation would increase the reimbursement rate for the care given to Medicare patients and a flat payment for facility costs from the Centers for Medicaid and Medicare Services.
Rural Emergency Hospital designations were established by the federal government under legislation spearheaded by Iowa’s senior Republican U.S. Sen. Chuck Grassley in December 2020.
Grassley lobbied the U.S. Department of Health and Human Services to implement and finalize regulations so that rural hospitals can benefit from the designation. Regulations were finalized by the federal government in November 2022.
Grassley, having grown up in rural Iowa, said the designation allows hospitals to adapt and continue serving their communities in an outpatient capacity as they face financial struggles.
Iowa Sen. Janet Petersen, D-Des Moines, argued the Senate should go one step further and increase Medicaid reimbursement rates for Rural Emergency Hospitals and Critical Access Hospitals. Critical Access Hospitals are determined by the U.S. Department of Health and Human Services and serve rural areas providing critical lifelines to rural communities. CAHs can become Rural Emergency Hospitals by downsizing and stopping inpatient care.
While the federal legislation championed by Grassley increased Medicare reimbursement rates, Medicaid reimbursement rates — which are controlled by the state — have remained stagnant for over a decade.
Iowa Democrats want to increase the state’s share of costs in maintaining rural hospitals by boosting Medicaid reimbursement rates, but Republicans voted against the measure Petersen introduced to raise those rates.
“If we want to save rural health care, we need to fund rural health care,” Petersen said during floor debate in the Iowa Senate on Feb. 15. “Iowa should put skin in the game to keep our community hospitals open.”
Map by Jami Martin-Trainor/The Daily Iowan
During the debate on the bill, state Sen. Mark Costello, R-Imogene, said the federal government will increase payments to these hospitals. However, the federal government only sets Medicare reimbursement rates, and states administer, pay, and set the reimbursement rates, while states for Medicaid services.
SF 75, introduced by Sen. Jeff Reichman, a Republican born and raised in Keokuk, passed unanimously on the Senate floor and was signed into law in March.

Assistant Director of Louisa County Ambulance Service Dan Conry drives an ambulance in Columbus Junction, Iowa on Friday, March 24, 2023.
Rural ambulance services left to fill gaps
When rural hospitals close, emergency medical services providers are left to carry the burden. With the majority of Iowa’s ambulance services run by volunteer departments, this can leave some rural patients without critical access to care.
According to a 2019 report by the Iowa Department of Public Health, 75 percent of Iowa’s emergency medical service providers are volunteers.
With Rural Emergency Hospital designations, Petersen said during floor debate on the bill in February that she worries patients who require a transfer to a larger facility might be stuck with a hefty ambulance bill, or the ambulance service might have to pick up the cost.
Petersen said Lee County’s ambulance service saw an increase of 60 minutes in average transport time and an increase of $750,000 in spending in the county’s general fund since the hospital in Keokuk closed its doors.
Low Medicaid reimbursement rates and lack of coverage for transfers from one hospital to another are to blame for the spike in spending because the ambulance service has had to make up the difference, Petersen said.
She introduced an amendment that would increase Medicaid reimbursement rates for ambulance providers transporting a patient from a rural facility to a larger inpatient facility. But the amendment failed on party lines, 15-33, with Democrats in favor.
“There are 17 to 21 rural hospitals [in Iowa] that could find themselves in the same circumstances that they’re facing in Lee County,” Petersen said. “If [a patient is] covered by Medicaid, Medicaid would pick up the cost of taking them by ambulance to a hospital where they can get the care they need and not have the cost of that hospital ride dumped on an Iowa family or dumped on property taxpayers.”

Dan Conry, Jen Martin and Jim Ingham adjusts a stretcher at the ambulance base in Columbus Junction, Iowa on Friday, March 24, 2023.
Experts: Creative solutions could help hospitals
As rural health care struggles to cope with financial pressures and some communities face losing access to vital health care resources, Keith Muller, the director of the Rural Policy Research Institute’s Center for Health Policy Analysis and University of Iowa professor of Health Management and Policy, said hospitals are using innovative financial strategies to stay afloat.
Muller said rural hospitals are reducing the number of services they provide and joining coalitions to spread out financial risk and impacts across multiple hospitals.
“So many [rural hospitals] have adopted or adapted by changing their service mix, by getting involved in regional networks doing other things that actually have improved their financial condition,” Muller said.
Technology also might be part of the solution to continued access to care.
During COVID-19, telehealth, video, or phone call appointments with health care professionals helped patients continue to access primary care when face-to-face appointments were not possible due to the efforts to curb the spread of the virus.
Telehealth didn’t fade with the pandemic; it flourished as a way for providers to connect with patients wherever they are.
Whitney Zahnd, a University of Iowa assistant professor of health management and policy, said telehealth is an innovative way to connect with rural patients and solve staffing shortages in rural hospitals, which many hospitals face on top of financial pressures.
Zahnd said the use of remote physician care is becoming increasingly popular. She said that larger, more urban hospitals in the state can help smaller rural facilities by consulting with physicians and patients via video conferencing to elevate the level of care offered at that facility.
“Those are a couple of examples on the hospital side that can help ensure that patients get the care they need and help prevent unnecessary transfers if they can get the care they need in the hospital they’re currently in,” Zahnd said.
Additionally, the expansion of the duties of some health care providers, such as physician assistants and advanced nurse practitioners, would help mend the health care worker shortage and create easier access to care for rural patients, Zahnd said.
“Expanding the scope of practice [for these providers] would allow for nurse practitioners and physician’s assistants to practice a little more independently with less oversight from physicians,” Zahnd said. “And those kinds of practitioners really provide a lot of care in rural areas.”